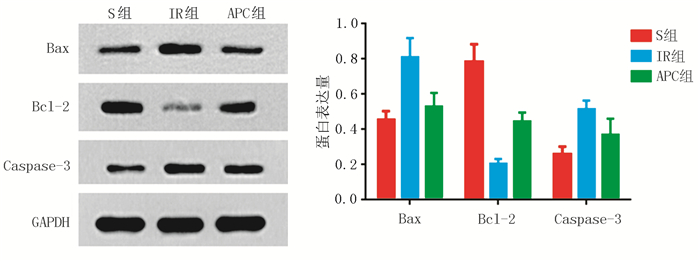
Effect of pretreatment with allopurinol on the expression of Bax, Bcl-2 and Caspase-3 in kidney of ischemia-reperfusion injury rats
-
摘要:
目的 探讨别嘌醇预处理对大鼠肾脏缺血-再灌注损伤(IRI)的影响及其机制。 方法 将24只SD大鼠随机分为3组:假手术组(S组)、缺血-再灌注组(IR组)、别嘌醇预处理组(APC组), 每组8只。手术前2周开始, 向APC组大鼠腹腔注射别嘌醇[50 mg/(kg·d)], 向S组及IR组大鼠腹腔注射等容量的生理盐水。预处理完成后S组切除右肾, IR组及APC组切除右肾并对左肾进行30 min缺血-再灌注处理。再灌注后24 h取血液标本, 术后2周取肾脏组织标本。采用全自动生化分析仪检测血尿素氮(BUN)和血清肌酐(Scr)水平。采用丙二醛(MDA)检测试剂盒与超氧化物歧化酶(SOD)活性检测试剂盒分别检测血浆MDA与总SOD活性水平。采用蛋白印迹法检测大鼠肾组织中Bax、Bcl-2和Caspase-3的表达水平。光学显微镜(光镜)下观察大鼠肾脏组织病理变化。采用dUTP缺口末端标记(TUNEL)染色法检测大鼠肾脏细胞凋亡情况。 结果 与S组比较, IR组及APC组大鼠BUN、Scr、血浆MDA水平均明显升高, 血浆SOD活性水平均明显降低; 与IR组比较, APC组BUN、Scr、血浆MDA水平均明显降低, 血浆SOD活性水平明显升高(均为P < 0.05)。与S组比较, IR组与APC组肾组织Bax和Caspase-3蛋白表达量均明显增加, APC组明显低于IR组(均为P < 0.05)。与S组比较, IR组与APC组肾组织Bcl-2蛋白表达量均明显降低, 但APC组明显高于IR组(均为P < 0.05)。光镜下, S组大鼠肾组织结构完整, 形态正常; IR组肾小管管腔明显扩张, 肾小管上皮细胞出现大量坏死, 间质水肿明显, 其内可见大量淋巴细胞浸润; APC组肾小管管腔轻度扩张, 肾间质未见明显水肿, 间质内少量淋巴细胞浸润。TUNEL染色结果显示, S组、IR组和APC组的肾脏细胞凋亡率分别为(4.1±1.7)%、(32.8±8.9)%、(12.6±3.4)%(均为P < 0.05)。 结论 别嘌醇预处理可能通过抗氧化作用抑制细胞凋亡, 从而减轻大鼠肾脏IRI, 改善肾功能。 Abstract:Objective To investigate the effect and mechanism of pretreatment with allopurinol on renal ischemia-reperfusion injury(IRI) in rats. Methods Twenty four rats were randomly assigned into the sham operation (S), ischemia-reperfusion (IR) and allopurinol pretreatment (APC) groups (n=8 for each group). At preoperative 2 weeks, allopurinol at a dose of 50 mg/(kg·d) was administered via intraperitoneal injection in the APC group, and an equivalent quantity of physiological saline was given via intraperitoneal injection in the S and IR groups. After pretreatment, the right kidneys of rats in the S group were resected. In the IR and APC groups, the right kidneys were resected and the left kidneys were treated with 30 min ischemia-reperfusion. Blood sample was collected at 24 h after reperfusion and the kidney specimen was obtained at postoperative 2 weeks. The levels of blood urea nitrogen (BUN) and serum creatinine (Scr) were detected by automatic biochemistry analyzer. The activity of plasma malondialdehyde (MDA) and superoxide dismutase (SOD) was respectively assessed by detection kits. The expression levels of Bax, Bcl-2 and Caspase-3 of rat kidney were measured by western blot. Pathological changes in the rat kidney were observed under light microscope. Cell apoptosis of rat kidney was evaluated by TdT mediated-dUTP nick end labeling (TUNEL). Results Compared with the S group, the levels of BUN, Scr and plasma MDA in the IR and APC groups were significantly increased, whereas the activity of plasma SOD was significantly reduced(all in P < 0.05). Compared with the IR group, the levels of BUN, Scr and plasma MDA in the APC group were significantly reduced, whereas the activity of plasma SOD was considerably elevated (all in P < 0.05). Compared with the S group, the expression levels of Bax and Caspase-3 proteins were significantly up-regulated in the IR and APC groups, and the levels in the APC group were considerably lower than those in the IR group (all in P < 0.05). Compared with the S group, the expression of Bcl-2 in rat kidney in the IR and APC groups was significantly down-regulated, and the value in the APC group was dramatically higher than that in the IR group (all in P < 0.05). Under light microscope, the morphology of rat kidney was intact and normal in the S group. In the IR group, evident renal tubular ectasia, massive necrosis of renal tubular epithelial cells, evident stromal edema and a large quantity of lymph cellular infiltration were observed. In the APC group, mild renal tubular ectasia was observed, whereas no apparent kidney stromal edema was noted. A slight amount of lymph cellular infiltration was noted in the stroma. TUNEL staining revealed that the apoptosis rate of kidney cells in the S, IR and APC groups was (4.1±1.7)%, (32.8±8.9)% and (12.6±3.4)% (all in P < 0.05). Conclusions Allopurinol pretreatment could suppress cell apoptosis through anti-oxidation effect, thereby alleviating IRI of rat kidney and improving renal function. -
Key words:
- Ischemia-reperfusion injury /
- Kidney /
- Rat /
- Allopurinol /
- Apoptosis /
- Renal function
-
表 1 各组大鼠术后24 h肾功能和血浆MDA及SOD活性水平的比较
Table 1. Comparison of renal function, the levels of MDA and SOD activity in plasma of rats in each group at 24 h after operation (x±s)
组别 n BUN(mmol/L) Scr(μmol/L) MDA(μmol/L) SOD(U/L) S组 8 7±2 27±4 7±1 43±12 IR组 8 15±4a 123±20a 10±2a 14±3a APC组 8 13±5a, b 91±13a, b 8±1a, b 28±5a, b 与S组比较,a P < 0.05;与IR组比较,b P < 0.05 -
[1] 乔良伟, 曲青山.传统尸体供肾与心脏死亡器官捐献供肾肾移植效果的比较[J].器官移植, 2013, 4(5): 284-287. http://www.organtranspl.com/browse/detail/qkid/66/id/271.htmlQiao LW, Qu QS. Comparison of the effect of renal transplantation between traditional cadaver donor and donation after cardiac death[J]. Organ Transplant, 2013, 4(5):284-287. http://www.organtranspl.com/browse/detail/qkid/66/id/271.html [2] 李小庆, 程颖, 刘强, 等.心脏死亡器官捐献供肾移植早期肾功能恢复情况的荟萃分析[J].中华器官移植杂志, 2013, 34(3):167-170. http://med.wanfangdata.com.cn/Paper/Detail/PeriodicalPaper_zhqgyz98201303011Li XQ, Cheng Y, Liu Q, et al. Meta-analysis of the early renal function recovery after kidney transplant from cardiac death donors[J]. Chin J Organ Transplant, 2013, 34(3):167-170. http://med.wanfangdata.com.cn/Paper/Detail/PeriodicalPaper_zhqgyz98201303011 [3] Lee WY, Koh EJ, Lee SM. A combination of ischemic preconditioning and allopurinol protects against ischemic injury through a nitric oxide-dependent mechanism[J]. Nitric Oxide, 2012, 26(1):1-8. doi: 10.1016/j.niox.2011.11.002 [4] Neuhof C, Neuhof H. Calpain system and its involvement in myocardial ischemia and reperfusion injury[J]. World J Cardiol, 2014, 6(7):638-652. doi: 10.4330/wjc.v6.i7.638 [5] Miyazawa K, Miyagi S, Maida K, et al. Edaravone, a free radical scavenger, improves the graft viability on liver transplantation from non-heart-beating donors in pigs[J]. Transplant Proc, 2014, 46(4):1090-1094. doi: 10.1016/j.transproceed.2013.11.155 [6] Jennings RB. Historical perspective on the pathology of myocardial ischemia/reperfusion injury[J]. Circ Res, 2013, 113(4):428-438. doi: 10.1161/CIRCRESAHA.113.300987 [7] Kaul S. The "no reflow" phenomenon following acute myocardial infarction: mechanisms and treatment options[J]. J Cardiol, 2014, 64(2):77-85. doi: 10.1016/j.jjcc.2014.03.008 [8] Gutowski M, Kowalczyk S. A study of free radical chemistry: their role and pathophysiological significance[J]. Acta Biochim Pol, 2013, 60(1):1-16. http://www.ncbi.nlm.nih.gov/pubmed/23513192 [9] Gormus ZI, Celik JB, Ergene N, et al. Does preoperative administration of allopurinol protect the lungs from ischemia-reperfusion injury occuring during cardiopulmonary bypass[J]. Bratisl Lek Listy, 2013, 114(10):561-565. http://www.ncbi.nlm.nih.gov/pubmed/24156678 [10] Rachmat FD, Rachmat J, Sastroasmoro S, et al. Effect of allopurinol on oxidative stress and hypoxic adaptation response during surgical correction of tetralogy of fallot[J]. Acta Med Indones, 2013, 45(2):94-100. https://www.researchgate.net/publication/239732567_Effect_of_allopurinol_on_oxidative_stress_and_hypoxic_adaptation_response_during_surgical_correction_of_tetralogy_of_fallot [11] Sapalidis K, Papavramidis TS, Gialamas E, et al. The role of allopurinol's timing in the ischemia reperfusion injury of small intestine[J]. J Emerg Trauma Shock, 2013, 6(3):203-208. doi: 10.4103/0974-2700.115346 [12] Renault TT, Teijido O, Antonsson B, et al. Regulation of Bax mitochondrial localization by Bcl-2 and Bcl-x(L): keep your friends close but your enemies closer[J]. Int J Biochem Cell Biol, 2013, 45(1):64-67. doi: 10.1016/j.biocel.2012.09.022 [13] Yang T, Zhang Y, Li Y, et al. High amounts of fluoride induce apoptosis/cell death in matured ameloblast-like LS8 cells by downregulating Bcl-2[J]. Arch Oral Biol, 2013, 58(9):1165-1173. doi: 10.1016/j.archoralbio.2013.03.016 [14] Renault TT, Manon S. Bax: addressed to kill[J]. Biochimie, 2011, 93(9):1379-1391. doi: 10.1016/j.biochi.2011.05.013 [15] Taeger CD, Müller-Seubert W, Horch RE, et al. Ischaemia-related cell damage in extracorporeal preserved tissue: new findings with a novel perfusion model[J]. J Cell Mol Med, 2014, 18(5):885-894. doi: 10.1111/jcmm.2014.18.issue-5 [16] Snigdha S, Smith ED, Prieto GA, et al. Caspase-3 activation as a bifurcation point between plasticity and cell death[J]. Neurosci Bull, 2012, 28(1):14-24. doi: 10.1007/s12264-012-1057-5 -





 下载:
下载: