Difference of clinical efficacy between surgical magnifying glass and surgical microscope assisted hepatic artery reconstruction in living donor liver transplantation
-
摘要:
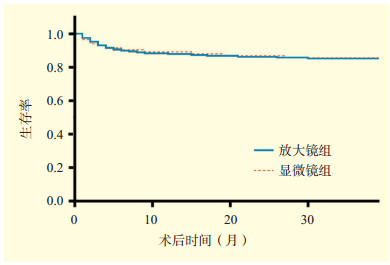
目的 探讨手术放大镜与手术显微镜辅助方式下行活体肝移植(LDLT)术中肝动脉重建的疗效差异。 方法 回顾性分析272例LDLT供、受者的临床资料。根据肝动脉重建方式不同将受者分为放大镜组(189例)和显微镜组(83例), 评估两组受者手术时间、术中出血量、肝动脉重建位置、吻合口直径、术后并发症发生率、受者生存率等的差异。 结果 与显微镜组比较, 放大镜组的总手术时间更短、肝动脉重建时间更短、术中出血量更少, 差异均有统计学意义(均为P < 0.001)。放大镜组及显微镜组行肝动脉重建的最常见位置均为肝右动脉, 吻合口直径分别为(2.1±0.9)mm、(2.1±0.8)mm, 两组比较差异无统计学意义(P > 0.05)。放大镜组和显微镜组受者术后1、2、3年生存率分别为88%、86%、85%和89%、87%、86%, 差异均无统计学意义(均为P > 0.05)。两组受者术后并发症发生率比较, 差异亦均无统计学意义(均为P > 0.05)。 结论 LDLT术中手术放大镜下行肝动脉重建的效果及安全性并不低于手术显微镜, 且手术工作量和术中出血量更少。对于经验丰富的移植外科医师, 建议在放大镜辅助下行肝动脉重建操作。 -
关键词:
- 活体肝移植 /
- 肝动脉重建 /
- 手术显微镜 /
- 手术用双目放大镜 /
- 围手术期 /
- 终末期肝病模型(MELD)评分 /
- Child-Pugh分级 /
- 肝动脉血栓
Abstract:Objective To compare the difference of clinical efficacy between surgical magnifying glass and surgical microscope assisted hepatic artery reconstruction in living donor liver transplantation (LDLT). Methods Clinical data of 272 donors and recipients undergoing LDLT were retrospectively analyzed. According to different patterns of hepatic artery reconstruction, all recipients were divided into the magnifying glass group (n=189) and microscope group (n=83). The operation time, intraoperative blood loss, hepatic artery reconstruction site, diameter of anastomosis, incidence of postoperative complications and survival rate of recipients were statistically compared between two groups. Results Compared with the microscope group, the operation time, hepatic artery reconstruction time and intraoperative blood loss were significantly less in the magnifying glass group (all P < 0.001). The most common site of hepatic artery reconstruction was the right hepatic artery in two groups, and the diameter of anastomosis was (2.1±0.9) mm in the magnifying glass group and (2.1±0.8) mm in the microscope group, with no statistical significance between two groups (P > 0.05). The 1-, 2- and 3-year survival rates of recipients in the magnifying glass group were 88%, 86% and 85%, which did not significantly differ from 89%, 87% and 86% in the microscope group (all P > 0.05). The incidence of postoperative complications did not significantly differ between two groups (all P > 0.05). Conclusions The efficacy and safety of hepatic artery reconstruction in LDLT under surgical magnifying glass are equivalent to those under surgical microscope, with less operation workload and intraoperative blood loss. For experienced transplantation surgeons, it is recommended to perform hepatic artery reconstruction assisted by surgical magnifying glass. -
表 1 两组受者手术时间和出血量的比较
Table 1. Comparison of operation time and bleeding volume of recipients between two groups (x±s)
组别 n 手术时间(h) 出血量(mL) 肝动脉重建时间(min) 放大镜组 189 6.8±0.9 395±139 19±4 显微镜组 83 7.3±1.1 462±151 25±6 P值 < 0.001 < 0.001 < 0.001 表 2 两组受者肝动脉重建位置的比较
Table 2. Comparison of the location of hepatic artery reconstruction of recipients between two groups [n(%)]
组别 n 肝固有动脉 肝右动脉 肝左动脉 其他 放大镜组 189 46(24) 115(61) 12(6) 16(8) 显微镜组 83 18(22) 54(65) 3(4) 8(10) P值 0.753 0.459 0.562 0.818 -
[1] BOZKURT B, DAYANGAC M, TOKAT Y. Living donor liver transplantation[J]. Chirurgia (Bucur), 2017, 112(3):217-228. DOI: 10.21614/chirurgia.112.3.217. [2] UCHIYAMA H, HASHIMOTO K, HIROSHIGE S, et al. Hepatic artery reconstruction in living-donor liver transplantation: a review of its techniques and complications[J]. Surgery, 2002, 131(1 Suppl):S200-S204. DOI: 10.1067/msy.2002.119577. [3] LUO Y, ZHAO D, ZHANG M, et al. Hepatic artery reconstruction using 3-in-1 segmental resection in pediatric living donor liver transplantation: a case report and literature review[J]. Transplant Proc, 2017, 49(7):1619-1623. DOI: 10.1016/j.transproceed.2017.01.076. [4] LEE CF, LU JC, ZIDAN A, et al. Microscope-assisted hepatic artery reconstruction in adult living donor liver transplantation-a review of 325 consecutive cases in a single center[J]. Clin Transplant, 2017, 31(2). DOI: 10.1111/ctr.12879. [5] YAGI T, SHINOURA S, UMEDA Y, et al. Surgical rationalization of living donor liver transplantation by abolition of hepatic artery reconstruction under a fixed microscope[J]. Clin Transplant, 2012, 26(6):877-883. DOI: 10.1111/j.1399-0012.2012.01651.x. [6] HERNANDEZ JA, MULLENS CL, AOYAMA JT, et al. Analysis of outcomes in living donor liver transplants involving reconstructive microsurgeons[J]. J Reconstr Microsurg, 2020, 36(3):223-227. DOI: 10.1055/s-0039-3401033. [7] EHANIRE T, SINGHAL D, MAST B, et al. Safety of microsurgery under loupes versus microscope: a head-to-head comparison of 2 surgeons with similar experiences[J]. Ann Plast Surg, 2018, 80(Suppl 6):S340-S342. DOI: 10.1097/SAP.0000000000001324. [8] HERRERO A, SOUCHE R, JOLY E, et al. Early hepatic artery thrombosis after liver transplantation: what is the impact of the arterial reconstruction type?[J]. World J Surg, 2017, 41(8):2101-2110. DOI: 10.1007/s00268-017-3989-4. [9] SNEIDERS D, HOUWEN T, PENGEL LHM, et al. Systematic review and Meta-analysis of posttransplant hepatic artery and biliary complications in patients treated with transarterial chemoembolization before liver transplantation[J]. Transplantation, 2018, 102(1):88-96. DOI: 10.1097/TP.0000000000001936. [10] KUTLUTURK K, SAHIN TT, KARAKAS S, et al. Early hepatic artery thrombosis after pediatric living donor liver transplantation[J]. Transplant Proc, 2019, 51(4):1162-1168. DOI: 10.1016/j.transproceed.2019.01.104. [11] PULITI REIGADA CH, DE ATAIDE EC, DE ALMEIDA PRADO MATTOSINHO T, et al. Hepatic artery thrombosis after liver transplantation: five-year experience at the State University of Campinas[J]. Transplant Proc, 2017, 49(4):867-870. DOI: 10.1016/j.transproceed.2017.01.056. [12] ZHANG H, QIAN S, LIU R, et al. Interventional treatment for hepatic artery thrombosis after liver transplantation[J]. J Vasc Interv Radiol, 2017, 28(8):1116-1122. DOI: 10.1016/j.jvir.2017.04.026. [13] COMPAGNON P, TOSO C. Selective retransplantation after late hepatic artery thrombosis[J]. Transpl Int, 2019, 32(5):470-472. DOI: 10.1111/tri.13411. [14] LUI SK, GARCIA CR, MEI X, et al. Re-transplantation for hepatic artery thrombosis: a national perspective[J]. World J Surg, 2018, 42(10):3357-3363. DOI: 10.1007/s00268-018-4609-7. [15] MORI K, NAGATA I, YAMAGATA S, et al. The introduction of microvascular surgery to hepatic artery reconstruction in living-donor liver transplantation-its surgical advantages compared with conventional procedures[J]. Transplantation, 1992, 54(2):263-268. DOI: 10.1097/00007890-199208000-00014. [16] ZUO KJ, DRAGINOV A, PANOSSIAN A, et al. Microvascular hepatic artery anastomosis in pediatric living donor liver transplantation: 73 consecutive cases performed by a single surgeon[J]. Plast Reconstr Surg, 2018, 142(6):1609-1619. DOI: 10.1097/PRS.0000000000005044. [17] PARK GC, MOON DB, KANG SH, et al. Overcoming hepatic artery thrombosis after living donor liver transplantations: an experience from Asan medical center[J]. Ann Transplant, 2019, 24:588-593. DOI: 10.12659/AOT.919650. [18] BALCI D, AHN CS. Hepatic artery reconstruction in living donor liver transplantation[J]. Curr Opin Organ Transplant, 2019, 24(5):631-636. DOI: 10.1097/MOT.0000000000000697. [19] FOUZAS I, PAPANIKOLAOU C, KATSANOS G, et al. Hepatic artery anatomic variations and reconstruction in liver grafts procured in Greece: the effect on hepatic artery thrombosis[J]. Transplant Proc, 2019, 51(2):416-420. DOI: 10.1016/j.transproceed.2019.01.078. [20] JWA EK, KIM JD, CHOI DL. Comparison of hepatic artery reconstruction using surgical loupe and operating microscope during living donor liver transplantation focusing on the beginner's point[J]. Ann Hepatobiliary Pancreat Surg, 2019, 23(2):122-127. DOI: 10.14701/ahbps.2019.23.2.122. [21] MARUBASHI S, KOBAYASHI S, WADA H, et al. Hepatic artery reconstruction in living donor liver transplantation: risk factor analysis of complication and a role of MDCT scan for detecting anastomotic stricture[J]. World J Surg, 2013, 37(11):2671-2677. DOI: 10.1007/s00268-013-2188-1. [22] OKOCHI M, OKOCHI H, SAKABA T, et al. Hepatic artery reconstruction in living donor liver transplantation: strategy of the extension of graft or recipient artery[J]. J Plast Surg Hand Surg, 2019, 53(4):216-220. DOI: 10.1080/2000656X.2019.1582426. [23] YAN S, ZHANG QY, YU YS, et al. Microsurgical reconstruction of hepatic artery in living donor liver transplantation: experiences and lessons[J]. Hepatobiliary Pancreat Dis Int, 2009, 8(6):575-580. [24] UCHIYAMA H, SHIRABE K, MORITA M, et al. Expanding the applications of microvascular surgical techniques to digestive surgeries: a technical review[J]. Surg Today, 2012, 42(2):111-120. DOI: 10.1007/s00595-011-0032-5. [25] VASCONCELOS-FILHO JM, MAGALHÃES PRM, MONTEIRO BR, et al. Frequency of anatomic variations on hepatic arteries and types of reconstruction employed: study on livers prepared for transplantation[J]. Transplant Proc, 2020, 52(5): 1312-1313. DOI: 10.1016/j.transproceed.2020.01.070. -





 下载:
下载: