-
摘要:
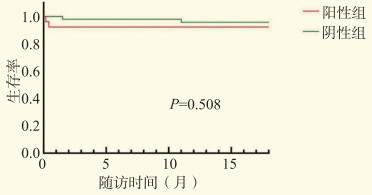
目的 探讨供者来源性感染对肝移植受者预后的影响。 方法 分析75例行肝移植供、受者临床资料。根据供者器官灌洗液培养结果,将受者分为阳性组(26例)和阴性组(49例)。观察阳性组和阴性组受者围手术期相关临床指标,对肝移植受者痰液、腹腔引流液进行培养,观察受者术后感染情况。采用Kaplan-Meier法分析受者术后1.5年的生存曲线。 结果 阳性组受者门静脉狭窄和门静脉血栓的发生率明显高于阴性组受者(P < 0.05)。75例肝移植受者中,发生术后感染者33例(44%),受者发生感染的部位以肺部和腹腔为主,阳性组和阴性组的感染率分别为77%、27%,差异有统计学意义(P < 0.05)。阳性组中,痰液、腹腔引流液培养阳性分别为10例、11例,其中4例受者痰培养结果与其供者器官灌洗液培养结果一致,6例受者腹腔引流液培养结果与其供者器官灌洗液培养结果一致。经过抗感染治疗后,阳性组中2例受者分别于术后5、12 d死亡,其余受者的培养结果均转阴。阴性组中,痰液、腹腔引流液培养阳性分别为7例、6例,经抗感染治疗后培养结果均转阴,2例受者因移植物肝衰竭分别于术后1个月、1年死亡。阳性组和阴性组受者移植术后1.5年生存率比较,差异无统计学意义(P > 0.05)。 结论 供者来源性感染对肝移植受者早期预后的影响不可忽视,但对中晚期预后影响不大。 Abstract:Objective To evaluate the effect of donor-derived infection on the clinical prognosis of the recipients undergoing liver transplantation. Methods Clinical data of 75 donors and recipients undergoing liver transplantation were retrospectively analyzed. According to the culture results of donor organ lavage fluid, all recipients were divided into the positive group (n=26) and negative group (n=49). Clinical parameters of the recipients during perioperative period were observed in the positive and negative groups. The sputum and peritoneal drainage fluid of the recipients undergoing liver transplantation were cultured. The incidence of postoperative infection of the recipients was observed. The 1.5-year survival curve of the recipients was analyzed by Kaplan-Meier method. Results In the positive group, the incidence of portal vein stenosis and thrombosis was significantly higher than that in the negative group (P < 0.05). Among 75 recipients undergoing liver transplantation, 33 cases (44%) developed postoperative infection mainly in the lung and abdominal cavity. The infection rate significantly differed between the positive group (77%) and negative group (27%, P < 0.05). In the positive group, sputum culture was positive in 10 recipients and peritoneal drainage culture was positive in 11 recipients. The sputum culture outcomes of 4 recipients were consistent with those of the organ lavage fluid culture of their donors. The peritoneal drainage culture results of 6 recipients were consistent with those of the organ lavage fluid culture of their donors. After anti-infection treatment, 2 recipients in the positive group died at postoperative 5 and 12 d, and the culture results of the remaining recipients were negative. In the negative group, 7 recipients were positive for sputum culture and 6 recipients were positive for peritoneal drainage culture. The culture results of all recipients were negative following anti-infection therapy. Two recipients died from graft failure at postoperative 1 month and 1 year. The 1.5-year survival rate did not significantly differ between the positive and negative groups (P > 0.05). Conclusions The effect of donor-derived infection on the early prognosis of liver transplant recipients cannot be neglected, whereas it exerts mild impact on the intermediate- and long-term clinical prognosis of the recipients. -
表 1 两组受者围手术期情况比较
Table 1. Comparison of perioperative status between two groups of recipients
指标 阳性组(n=26) 阴性组(n=49) P值 手术时间(min,x±s) 436±109 400±106 > 0.05 术中出血量[mL, M(R)] 700(4 350) 900(1 820) > 0.05 住院时间[d, M(R)] 16(133) 19(56) > 0.05 ICU住院时间[d, M(R)] 3(32) 4(7) > 0.05 术后胆道、血管性并发症[n(%)] 胆漏、胆道狭窄 0(0) 1(2) > 0.05 门静脉狭窄、门静脉血栓 4(15) 0(0) < 0.05 肝动脉闭塞 2(8) 3(6) > 0.05 死亡[n(%)] 2(8) 1(2) > 0.05 -
[1] ECHENIQUE IA, ISON MG. Update on donor-derived infections in liver transplantation[J]. Liver Transpl, 2013, 19(6):575-585. DOI: 10.1002/lt.23640. [2] CHAN KM, CHENG CH, WU TH, et al. Impact of donor with evidence of bacterial infections on deceased donor liver transplantation: a retrospective observational cohort study in Taiwan[J]. BMJ Open, 2019, 9(3):e023908. DOI: 10.1136/bmjopen-2018-023908. [3] 朱有华.DCD供者来源感染现状与防控策略[J/CD].实用器官移植电子杂志, 2018, 6(1): 49-50. DOI: 10.3969/j.issn.2095-5332.2018.01.012.ZHU YH. Current situation and prevention and control strategy of DCD donor-derived infection[J/CD]. Pract J Organ Transplant (Electr Vers), 2018, 6(1): 49-50. DOI: 10.3969/j.issn.2095-5332.2018.01.012. [4] ABAD CL, LAHR BD, RAZONABLE RR. Epidemiology and risk factors for infection after living donor liver transplantation[J]. Liver Transpl, 2017, 23(4):465-477. DOI: 10.1002/lt.24739. [5] VERA A, CONTRERAS F, GUEVARA F. Incidence and risk factors for infections after liver transplant: single-center experience at the University Hospital Fundación Santa Fe de Bogotá, Colombia[J]. Transpl Infect Dis, 2011, 13(6):608-615. DOI: 10.1111/j.1399-3062.2011.00640.x. [6] ROMERO FA, RAZONABLE RR. Infections in liver transplant recipients[J]. World J Hepatol, 2011, 3(4):83-92. DOI: 10.4254/wjh.v3.i4.83. [7] FISHMAN JA. Infection in solid-organ transplant recipients[J]. N Engl J Med, 2007, 357(25):2601-2614. doi: 10.1056/NEJMra064928 [8] SANTORO-LOPES G, DE GOUVÊA EF. Multidrug-resistant bacterial infections after liver transplantation: an ever-growing challenge[J]. World J Gastroenterol, 2014, 20(20):6201-6210. DOI: 10.3748/wjg.v20.i20.6201. [9] CAMARGO JF. Donor-derived infections in solid organ transplant recipients: challenging the 30-day paradigm[J]. Transpl Infect Dis, 2017, 19(2). DOI: 10.1111/tid.12665. [10] FISCHER SA. Is this organ donor safe?: donor-derived infections in solid organ transplantation[J]. Surg Clin North Am, 2019, 99(1):117-128. DOI: 10.1016/j.suc.2018.09.009. [11] ANGELIS M, COOPER JT, FREEMAN RB. Impact of donor infections on outcome of orthotopic liver transplantation[J]. Liver Transpl, 2003, 9(5):451-462. doi: 10.1053/jlts.2003.50094 [12] 李海波, 符洪源, 陆桐宇, 等.肝移植领域2017年度重要进展盘点[J].器官移植, 2018, 9(1):41-50, 82. DOI: 10.3969/j.issn.1674-7445.2018.01.006.LI HB, FU HY, LU TY, et al. Summary of important research on liver transplantation in 2017 [J]. Organ Transplant, 2018, 9(1):41-50, 82. DOI:10.3969/j.issn.1674- 7445.2018.01.006. [13] YE QF, ZHOU W, WAN QQ. Donor-derived infections among Chinese donation after cardiac death liver recipients[J]. World J Gastroenterol, 2017, 23(31):5809-5816. DOI: 10.3748/wjg.v23.i31.5809. [14] NERY JR, WEPPLER D, KETCHUM P, et al. Donor infection and primary nonfunction in liver transplantation[J]. Transplant Proc, 1997, 29(1/2):481-483. doi: 10.1016/S0041-1345(96)00214-X [15] BIGAT Z, HADIMIOGLU N, ERTUG Z, et al. Spinal analgesia for the postoperative period in renal donors[J]. Transplant Proc, 2006, 38(2):392-395. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=0ec5f0ffd771e8c60c8597b1386f4728 [16] ORIOL I, SABÉ N, TEBÉ C, et al. Clinical impact of culture-positive preservation fluid on solid organ transplantation: a systematic review and Meta-analysis[J]. Transplant Rev (Orlando), 2018, 32(2):85-91. DOI: 10.1016/j.trre.2017.11.003. [17] YANSOUNI CP, DENDUKURI N, LIU G, et al. Positive cultures of organ preservation fluid predict postoperative infections in solid organ transplantation recipients[J]. Infect Control Hosp Epidemiol, 2012, 33(7):672-680. DOI: 10.1086/666344. [18] CERUTTI E, STRATTA C, ROMAGNOLI R, et al. Bacterial- and fungal-positive cultures in organ donors: clinical impact in liver transplantation[J]. Liver Transpl, 2006, 12(8):1253-1259. doi: 10.1002/lt.20811 [19] GARZONI C, ISON MG. Uniform definitions for donor-derived infectious disease transmissions in solid organ transplantation[J]. Transplantation, 2011, 92(12):1297-1300. DOI: 10.1097/TP.0b013e318236cd02. [20] WOLFE CR, ISON MG, AST Infectious Diseases Community of Practice. Donor-derived infections: guidelines from the American Society of Transplantation Infectious Diseases Community of Practice[J]. Clin Transplant, 2019:e13547. DOI: 10.1111/ctr.13547. [21] NAM H, NILLES KM, LEVITSKY J, et al. Donor-derived viral infections in liver transplantation[J]. Transplantation, 2018, 102(11):1824-1836. DOI: 10.1097/TP.0000000000002326. [22] KIRCHNER VA, PRUETT TL. Receiving the unwanted gift: infection transmission through organ transplantation[J]. Surg Infect (Larchmt), 2016, 17(3):318-322. DOI: 10.1089/sur.2016.009. [23] LEWIS JD, SIFRI CD. Multidrug-resistant bacterial donor-derived infections in solid organ transplantation[J]. Curr Infect Dis Rep, 2016, 18(6):18. DOI: 10.1007/s11908-016-0526-9. [24] BARTOLETTI M, GIANNELLA M, TEDESCHI S, et al. Multidrug-resistant bacterial infections in solid organ transplant candidates and recipients[J]. Infect Dis Clin North Am, 2018, 32(3):551-580. DOI: 10.1016/j.idc.2018.04.004. [25] CERVERA C, VAN DELDEN C, GAVALDÀ J, et al. Multidrug-resistant bacteria in solid organ transplant recipients[J]. Clin Microbiol Infect, 2014, 20(Suppl 7):49-73. DOI: 10.1111/1469-0691.12687. -





 下载:
下载: